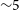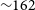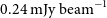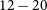23 results
The experiences of familial mental illness stigma among individuals living with mental illnesses
- Joseph Adu, Abram Oudshoorn, Kelly Anderson, Carrie Anne Marshall, Heather Stuart
-
- Journal:
- Journal of Biosocial Science , First View
- Published online by Cambridge University Press:
- 17 April 2024, pp. 1-22
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Persons with mental illnesses may experience stigma from their immediate family members in addition to other forms of stigma. Using semi-structured interviews, we investigated experiences of familial mental illness stigma among 15 people diagnosed with mental illnesses in a mid-sized city in Canada. We identified five themes that speak to participants’ experiences of familial mental illness stigma and ways to reduce it. The themes include the following: diagnosis as a ‘double-edged sword,’ potential familial isolation, familial stigma as societal stigma localized, stories of acceptance, and confronting potential familial mental illness stigma. Participants’ narratives indicate that familial mental illness stigma is rooted in the broader social or public stigma, which sees its way into familial relations as well. This stigma takes various forms, including relationship bias or unfair treatment, breakdown in romantic relationships, loss of status, verbal and emotional abuse, exclusion from decision-making, and alienation within their immediate and extended families. Familial mental illness stigma experiences negatively impact participant’s psychological well-being and personal empowerment. However, participants also shared ways that family members create supportive environments or actively confront or prevent stigma. Overall, this study has contributed to knowledge on mental illness stigma, particularly familial mental illness stigma from the perspective of participants living with a mental illness in a high-income country. Suggestions for future research include a focus on strategies to prevent ongoing familial mental illness stigma and large-scale studies to explore familial mental illness stigma to understand why families might perpetrate stigma.
“The Only Way Is Up; Lets Do It!”- a Quality Improvement Project for Physical Health Improvement for Patients Diagnosed With Schizophrenia at a CMHT in Glasgow Using Smart Interventions
- Brooke Marron, Lindsay Anderson, Fahd Cheema, Eleanor Dow, Stuart Hutchison, Marcel Kazmierczyk, Jasmeet Bindra, Jonathan Dourish, Julie Richardson
-
- Journal:
- BJPsych Open / Volume 9 / Issue S1 / July 2023
- Published online by Cambridge University Press:
- 07 July 2023, pp. S100-S101
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Aims
Cardiovascular death is the leading cause of early mortality in patients with schizophrenia. We audited physical health monitoring (via Lester tool) of all patients diagnosed with schizophrenia over the past year. There were 163 patients, 60% were up-to-date on blood tests, but only 28% had an up-to-date ECG. We found poor documentation of lifestyle risk factors (smoking/alcohol/weight) and recording of interventions that were offered to modify these. We felt it was important to try a pro-active model of engagement and intervention in order to improve outcomes and empower patients in collaboration with GPs.
MethodsA subset of the cohort (35 patients) were invited along for an all-inclusive check up with a doctor at the psychiatry clinic (blood tests, discussion and advice regarding lifestyle risk factors and on-site ECG utilising the new Kardia 6L) lasting 30 minutes. Information was collated and then distributed via a letter to the GP, the consultant psychiatrist and the patient.
ResultsOf the 35 patients invited to attend the physical health check-up, 18 (51%) attended. All patients then underwent physical health monitoring and discussion of how to improve their risk factors. The Kardia6L allowed for QTc monitoring to occur quickly and easily in the outpatient setting and was liked and accepted by patients. We found that most patients were overweight (88%) and were undertaking less than 30 minutes of exercise a day (50%). Half of the patients required active medical intervention (statin, blood pressure or diabetes medication). The Kardia6L allowed us to attain 88% compliance with achieving up-to-date ECGs and provided instant results to the clinicians/patients.
ConclusionIn this first phase of the quality improvement project we were able to show that half of the patients were willing to attend for in person monitoring. Patient engagement was better as intervention was being delivered at their usual CMHT by their Psychiatrists. The model of a shared letter between patient, GP and psychiatry encouraged shared responsibility for carrying these issues forward. From participating in the project the psychiatry team plan to review patient's medication and develop a robust intervention plan regarding weight loss/exercise/diet from the CMHT in collaboration with GPs as there are clear issues affecting our patient's health long term. The Kardia6L proved to be a quick/easy way to monitor QTc safely in an outpatient setting and allowed us to provide this as one step process at CMHT without requiring referral to Cardiology while improving compliance with annual ECGs.
The relationship between sleep and depression and bipolar disorder in children and young people
- Monica Comsa, Kirstie N. Anderson, Aditya Sharma, Vanishri C. Yadav, Stuart Watson
-
- Journal:
- BJPsych Open / Volume 8 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 14 January 2022, e27
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Sleep difficulties are often reported in practice, and are part of the diagnostic criteria for depression and bipolar disorder.
AimsTo inform the understanding of the relationship between sleep and both depression and bipolar disorder.
MethodWe conducted a narrative literature review of affective disorders and sleep difficulties in children and young people.
ResultsSpecific sleep disorders, such as parasomnias, narcolepsy and sleep-related movement disorders, are associated with depression, whereas insomnia, obstructive sleep apnoea and circadian rhythm disorders are associated with both depression and bipolar disorder in children and young people. Conversely, children and young people with depression can present with a number of sleep difficulties, and these are associated with higher depression severity and greater fatigue, suicidal ideation, physical complaints, pain and decreased concentration. Sleep disturbances among adolescents with bipolar disorder can affect the severity of depressive and manic symptoms, are a poor prognostic indicator and have been associated with social and academic impairment. Antidepressants and antipsychotics can directly affect sleep architecture, which clinicians need to be aware of. Non-pharmacological interventions for sleep problems could prevent and/or minimise the risk of relapse in affective disorders.
ConclusionsSleep difficulties can occur before, during and after an episode of depression or bipolar disorder, and have a higher prevalence in affective disorders compared with the general population. A multi-modal approach would include the treatment of both the affective and specific sleep disorder. Further research is needed in this field to understand the impact of combined interventions on clinical outcomes.
The ASKAP Variables and Slow Transients (VAST) Pilot Survey
- Part of
- Tara Murphy, David L. Kaplan, Adam J. Stewart, Andrew O’Brien, Emil Lenc, Sergio Pintaldi, Joshua Pritchard, Dougal Dobie, Archibald Fox, James K. Leung, Tao An, Martin E. Bell, Jess W. Broderick, Shami Chatterjee, Shi Dai, Daniele d’Antonio, Gerry Doyle, B. M. Gaensler, George Heald, Assaf Horesh, Megan L. Jones, David McConnell, Vanessa A. Moss, Wasim Raja, Gavin Ramsay, Stuart Ryder, Elaine M. Sadler, Gregory R. Sivakoff, Yuanming Wang, Ziteng Wang, Michael S. Wheatland, Matthew Whiting, James R. Allison, C. S. Anderson, Lewis Ball, K. Bannister, D. C.-J. Bock, R. Bolton, J. D. Bunton, R. Chekkala, A. P Chippendale, F. R. Cooray, N. Gupta, D. B. Hayman, K. Jeganathan, B. Koribalski, K. Lee-Waddell, Elizabeth K. Mahony, J. Marvil, N. M. McClure-Griffiths, P. Mirtschin, A. Ng, S. Pearce, C. Phillips, M. A. Voronkov
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 38 / 2021
- Published online by Cambridge University Press:
- 12 October 2021, e054
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The Variables and Slow Transients Survey (VAST) on the Australian Square Kilometre Array Pathfinder (ASKAP) is designed to detect highly variable and transient radio sources on timescales from 5 s to
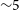 $\sim\!5$
yr. In this paper, we present the survey description, observation strategy and initial results from the VAST Phase I Pilot Survey. This pilot survey consists of
$\sim\!5$
yr. In this paper, we present the survey description, observation strategy and initial results from the VAST Phase I Pilot Survey. This pilot survey consists of 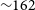 $\sim\!162$
h of observations conducted at a central frequency of 888 MHz between 2019 August and 2020 August, with a typical rms sensitivity of
$\sim\!162$
h of observations conducted at a central frequency of 888 MHz between 2019 August and 2020 August, with a typical rms sensitivity of 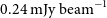 $0.24\ \mathrm{mJy\ beam}^{-1}$
and angular resolution of
$0.24\ \mathrm{mJy\ beam}^{-1}$
and angular resolution of 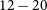 $12-20$
arcseconds. There are 113 fields, each of which was observed for 12 min integration time, with between 5 and 13 repeats, with cadences between 1 day and 8 months. The total area of the pilot survey footprint is 5 131 square degrees, covering six distinct regions of the sky. An initial search of two of these regions, totalling 1 646 square degrees, revealed 28 highly variable and/or transient sources. Seven of these are known pulsars, including the millisecond pulsar J2039–5617. Another seven are stars, four of which have no previously reported radio detection (SCR J0533–4257, LEHPM 2-783, UCAC3 89–412162 and 2MASS J22414436–6119311). Of the remaining 14 sources, two are active galactic nuclei, six are associated with galaxies and the other six have no multi-wavelength counterparts and are yet to be identified.
$12-20$
arcseconds. There are 113 fields, each of which was observed for 12 min integration time, with between 5 and 13 repeats, with cadences between 1 day and 8 months. The total area of the pilot survey footprint is 5 131 square degrees, covering six distinct regions of the sky. An initial search of two of these regions, totalling 1 646 square degrees, revealed 28 highly variable and/or transient sources. Seven of these are known pulsars, including the millisecond pulsar J2039–5617. Another seven are stars, four of which have no previously reported radio detection (SCR J0533–4257, LEHPM 2-783, UCAC3 89–412162 and 2MASS J22414436–6119311). Of the remaining 14 sources, two are active galactic nuclei, six are associated with galaxies and the other six have no multi-wavelength counterparts and are yet to be identified.
Peer mentoring in psychiatry: a trainee-led initiative
- Zoe Moore, Linda Irwin, Stuart Brown, Julie Anderson, Stephen Moore
-
- Journal:
- BJPsych Open / Volume 7 / Issue S1 / June 2021
- Published online by Cambridge University Press:
- 18 June 2021, p. S149
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Aims
Our aim was to establish a Peer Mentoring Network within Psychiatry Training in Northern Ireland.
Recognising that starting a new job can be a stressful time in any junior doctor's career, we wanted to ensure that new Core Trainees (CT1s) joining our Specialty Programme were well supported through this transition.
Although Clinical and Educational Supervision is well established in providing a support structure for trainees, we believed that a peer mentoring relationship, (with allocation of a Higher Psychiatry Trainee as mentor), would be of additional benefit.
It was hoped that the scheme would prove mutually beneficial to both mentee and mentor.
MethodWe delivered a presentation at CT1 induction and sent out follow-up emails to encourage participation. Higher trainees were also sent information via email and asked to complete a basic application form if interested in becoming a mentor. Prospective mentors then attended a one-day training session.
Two lead mentors, (also higher trainees), were allocated to oversee the scheme, with additional supervision from two lead Consultants. Mentor-Mentee matches were made based on information such as location, sub-specialty affiliations and outside interests.
Matched pairs were advised about the intended frequency and nature of contacts. Check-in emails were sent halfway through the year and feedback evaluations completed at the end.
Result95% of trainees who completed the evaluations said they would recommend the scheme to colleagues.
Mentees reported benefits in terms of personal and professional development, whilst mentors reported improved listening, coaching, and supervisory skills.
A small number of trainees highlighted that 6 monthly rotations impacted on ability to maintain face to face contacts.
Recruitment and engagement have improved annually. We are currently running the third year of the scheme and have achieved 100% uptake amongst CT1s and are over-subscribed with mentors, (19 mentors to 13 mentees).
ConclusionThe majority of feedback received has been positive and interest in the scheme continues to grow.
Potential issues relating to location of postings has been overcome, at least in part, by recent changes to ways of working and the use of alternative forms of contact, such as video calling.
Having exceeded demand in terms of mentor recruitment, we hope to extend the scheme to include trainees of other grades, and particularly those who are new to Northern Ireland.
We are excited to see where the next stage of our journey takes us and hope that others will be inspired to embark on similar schemes within their areas of work.
A pilot to assess the feasibility and potential clinical utility of enhanced sleep management on inpatient wards in a mental health trust
- Ambrina Roshi, Rose McGowan, Lauren Roberts, Stuart Watson, Kirstie Anderson, Patrick Keown, Rod Bowles, Ron Weddle, Sophie Connolly
-
- Journal:
- BJPsych Open / Volume 7 / Issue S1 / June 2021
- Published online by Cambridge University Press:
- 18 June 2021, p. S215
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Aims
To assess the feasibility and utility of introducing the following changes on to in-patient units:
Structural and cultural adaptation to create a sleep friendly ward environment
A “Protected Sleep Time” between midnight and 6am
Routine screening for sleep disorders, including obstructive sleep apnoea and restless leg syndrome
BackgroundInsomnia and other sleep disturbances are cause, correlate and consequence of psychiatric disorders. Routine hourly night time observations, ward noise, bright lights at night time, sleep disorders, insufficient exercise, insufficient day light exposure, too much caffeine and inappropriate psychotropic use are all causes of disturbed sleep (Horne 2018).
MethodSeven wards participated in a pilot (SleepWell). These consisted of one male and two female Acute Wards (General Adult), a High Dependency Unit, a Neurorehabilitation ward, an in-patient dementia service and one rehabilitation ward. These wards were supported via an existing trust management structure and the pilot was specifically supported by two trust managers (RW and RB) and by a clinical director (PK). The expectation was that each ward would identify a sleep champion from existing staff to facilitate the changes. A “product” was developed which identified core sleep management features but, in addition, wards were not confined to these. The existing policy that all inpatients should be checked each hour over night was suspended for the pilot wards and the patients had protected sleep time (PST) if the MDT agreed that it was clinically appropriate.
Quantitative and qualitative techniques were used to identify facilitators of change, impact on sleep and, outcome.
ResultProtected sleep was viewed positively by all staff and approximately 50% of patients on the pilot wards were able to have PST at some point in their admission. Routine sleep disorder assessments were harder to implement and 33% of patients were screened. There were no deaths or significant events on patients due to PST. Hypnotic use on the pilot wards reduced. It is anticipated that PST where it is safe will be rolled out across all adult and old age wards in the trust.
ConclusionWith support, it has been feasible to change many aspects of sleep management across a breadth of inpatient units in a large NHS trust.
The Smarter Sleep educational interventions: an initiative to reduce hypnotic prescribing in in-patient psychiatric care
- Alastair Paterson, Martina Khundakar, Anthony Young, Jonathan Ling, Samantha Chakraborty, Adam Pattison Rathbone, Stuart Watson, Tim Donaldson, Kirstie N. Anderson
-
- Journal:
- BJPsych Bulletin / Volume 46 / Issue 4 / August 2022
- Published online by Cambridge University Press:
- 05 May 2021, pp. 242-250
- Print publication:
- August 2022
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims and method
In-patients on mental health wards are commonly prescribed hypnotics for the long-term management of disturbed sleep. Specific sleep disorders remain underdiagnosed and effective behavioural interventions are underused. We developed a suite of three educational interventions (a video, poster and handbook) about sleep, sleep disorders, the safe prescribing of hypnotics and use of psychological strategies (sleep hygiene and cognitive–behavioural therapy for insomnia, CBTi) using co-design and multiprofessional stakeholder involvement. This controlled before-and-after study evaluated the effectiveness of these interventions across seven in-patient psychiatric wards, examining their impact on hypnotic prescribing rates and staff confidence scores (data collected by retrospective drug chart analysis and survey respectively).
ResultsA marked reduction was seen in the percentage of patients prescribed hypnotics on in-patient prescription charts (−24%), with a 41% reduction in the number of hypnotics administered per patient (mean reduction −1.142 administrations/patient).
Clinical implicationsThese simple educational strategies about the causes and treatment of insomnia can reduce hypnotic prescribing rates and increase staff confidence in both the medical and psychological management of insomnia.
Feasibility and utility of enhanced sleep management on in-patient psychiatry wards
- Part of
- Chloe Novak, Emma Packer, Alastair Paterson, Ambrina Roshi, Rosie Locke, Patrick Keown, Stuart Watson, Kirstie N. Anderson
-
- Journal:
- BJPsych Bulletin / Volume 44 / Issue 6 / December 2020
- Published online by Cambridge University Press:
- 24 April 2020, pp. 255-260
- Print publication:
- December 2020
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims and method
Sleep disturbance is common in psychiatry wards despite poor sleep worsening mental health. Contributory factors include the ward environment, frequent nightly checks on patients and sleep disorders including sleep apnoea. We evaluated the safety and feasibility of a package of measures to improve sleep across a mental health trust, including removing hourly checks when safe, sleep disorder screening and improving the ward environment.
ResultsDuring the pilot there were no serious adverse events; 50% of in-patients were able to have protected overnight sleep. Hypnotic issuing decreased, and feedback from patients and staff was positive. It was possible to offer cognitive–behavioural therapy for insomnia to selected patients.
Clinical implicationsMany psychiatry wards perform standardised, overnight checks, which are one cause of sleep disruption. A protected sleep period was safe and well-tolerated alongside education about sleep disturbance and mental health. Future research should evaluate personalised care rather than blanket observation policies.
Associations between childhood maltreatment and inflammatory markers
- Alish B. Palmos, Stuart Watson, Tom Hughes, Andreas Finkelmeyer, R. Hamish McAllister-Williams, Nicol Ferrier, Ian M. Anderson, Rajesh Nair, Allan H. Young, Rebecca Strawbridge, Anthony J. Cleare, Raymond Chung, Souci Frissa, Laura Goodwin, Matthew Hotopf, Stephani L. Hatch, Hong Wang, David A. Collier, Sandrine Thuret, Gerome Breen, Timothy R. Powell
-
- Journal:
- BJPsych Open / Volume 5 / Issue 1 / January 2019
- Published online by Cambridge University Press:
- 04 January 2019, e3
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Childhood maltreatment is one of the strongest predictors of adulthood depression and alterations to circulating levels of inflammatory markers is one putative mechanism mediating risk or resilience.
AimsTo determine the effects of childhood maltreatment on circulating levels of 41 inflammatory markers in healthy individuals and those with a major depressive disorder (MDD) diagnosis.
MethodWe investigated the association of childhood maltreatment with levels of 41 inflammatory markers in two groups, 164 patients with MDD and 301 controls, using multiplex electrochemiluminescence methods applied to blood serum.
ResultsChildhood maltreatment was not associated with altered inflammatory markers in either group after multiple testing correction. Body mass index (BMI) exerted strong effects on interleukin-6 and C-reactive protein levels in those with MDD.
ConclusionsChildhood maltreatment did not exert effects on inflammatory marker levels in either the participants with MDD or the control group in our study. Our results instead highlight the more pertinent influence of BMI.
Declaration of interestD.A.C. and H.W. work for Eli Lilly Inc. R.N. has received speaker fees from Sunovion, Jansen and Lundbeck. G.B. has received consultancy fees and funding from Eli Lilly. R.H.M.-W. has received consultancy fees or has a financial relationship with AstraZeneca, Bristol-Myers Squibb, Cyberonics, Eli Lilly, Ferrer, Janssen-Cilag, Lundbeck, MyTomorrows, Otsuka, Pfizer, Pulse, Roche, Servier, SPIMACO and Sunovian. I.M.A. has received consultancy fees or has a financial relationship with Alkermes, Lundbeck, Lundbeck/Otsuka, and Servier. S.W. has sat on an advisory board for Sunovion, Allergan and has received speaker fees from Astra Zeneca. A.H.Y. has received honoraria for speaking from Astra Zeneca, Lundbeck, Eli Lilly, Sunovion; honoraria for consulting from Allergan, Livanova and Lundbeck, Sunovion, Janssen; and research grant support from Janssen. A.J.C. has received honoraria for speaking from Astra Zeneca, honoraria for consulting with Allergan, Livanova and Lundbeck and research grant support from Lundbeck.
An evaluation of sleep disturbance on in-patient psychiatric units in the UK
- Part of
- Sam Horne, Katherine Hay, Stuart Watson, Kirstie N. Anderson
-
- Journal:
- BJPsych Bulletin / Volume 42 / Issue 5 / October 2018
- Published online by Cambridge University Press:
- 21 June 2018, pp. 193-197
- Print publication:
- October 2018
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims and method
Sleep disturbance is common on in-patient psychiatry wards. This study explored subjective and objective patterns of sleep disturbance and contributory environmental factors. Participants were recruited from mental health acute admission wards and had a range of subjective and objective assessments of sleep. Light intensity and noise levels were measured to characterise potential environmental causes for poor sleep.
ResultsWe recruited 20 patients; 15% were high risk for obstructive sleep apnoea. Nineteen participants reported poor sleep quality on the Pittsburgh Sleep Quality Index, and 90% had significant sleep fragmentation with objective measures. Inside light levels were low (day <200 lux and night <10 lux). Night sound levels were 40–90 db.
Clinical implicationsSleep disturbance was highly prevalent. Increased awareness of sleep disorders is needed. Modifiable environmental factors on the ward were implicated, therefore increased awareness and a change of approach to sleep disturbance in in-patient psychiatry is recommended.
Declaration of interestNone.
Contributors
-
- By Brittany L. Anderson-Montoya, Heather R. Bailey, Carryl L. Baldwin, Daphne Bavelier, Jameson D. Beach, Jeffrey S. Bedwell, Kevin B. Bennett, Richard A. Block, Deborah A. Boehm-Davis, Corey J. Bohil, David B. Boles, Avinoam Borowsky, Jessica Bramlett, Allison A. Brennan, J. Christopher Brill, Matthew S. Cain, Meredith Carroll, Roberto Champney, Kait Clark, Nancy J. Cooke, Lori M. Curtindale, Clare Davies, Patricia R. DeLucia, Andrew E. Deptula, Michael B. Dillard, Colin D. Drury, Christopher Edman, James T. Enns, Sara Irina Fabrikant, Victor S. Finomore, Arthur D. Fisk, John M. Flach, Matthew E. Funke, Andre Garcia, Adam Gazzaley, Douglas J. Gillan, Rebecca A. Grier, Simen Hagen, Kelly Hale, Diane F. Halpern, Peter A. Hancock, Deborah L. Harm, Mary Hegarty, Laurie M. Heller, Nicole D. Helton, William S. Helton, Robert R. Hoffman, Jerred Holt, Xiaogang Hu, Richard J. Jagacinski, Keith S. Jones, Astrid M. L. Kappers, Simon Kemp, Robert C. Kennedy, Robert S. Kennedy, Alan Kingstone, Ioana Koglbauer, Norman E. Lane, Robert D. Latzman, Cynthia Laurie-Rose, Patricia Lee, Richard Lowe, Valerie Lugo, Poornima Madhavan, Leonard S. Mark, Gerald Matthews, Jyoti Mishra, Stephen R. Mitroff, Tracy L. Mitzner, Alexander M. Morison, Taylor Murphy, Takamichi Nakamoto, John G. Neuhoff, Karl M. Newell, Tal Oron-Gilad, Raja Parasuraman, Tiffany A. Pempek, Robert W. Proctor, Katie A. Ragsdale, Anil K. Raj, Millard F. Reschke, Evan F. Risko, Matthew Rizzo, Wendy A. Rogers, Jesse Q. Sargent, Mark W. Scerbo, Natasha B. Schwartz, F. Jacob Seagull, Cory-Ann Smarr, L. James Smart, Kay Stanney, James Staszewski, Clayton L. Stephenson, Mary E. Stuart, Breanna E. Studenka, Joel Suss, Leedjia Svec, James L. Szalma, James Tanaka, James Thompson, Wouter M. Bergmann Tiest, Lauren A. Vassiliades, Michael A. Vidulich, Paul Ward, Joel S. Warm, David A. Washburn, Christopher D. Wickens, Scott J. Wood, David D. Woods, Motonori Yamaguchi, Lin Ye, Jeffrey M. Zacks
- Edited by Robert R. Hoffman, Peter A. Hancock, University of Central Florida, Mark W. Scerbo, Old Dominion University, Virginia, Raja Parasuraman, George Mason University, Virginia, James L. Szalma, University of Central Florida
-
- Book:
- The Cambridge Handbook of Applied Perception Research
- Published online:
- 05 July 2015
- Print publication:
- 26 January 2015, pp xi-xiv
-
- Chapter
- Export citation
The Evolving Landscape of Healthcare-Associated Infections: Recent Advances in Prevention and a Road Map for Research
- Nasia Safdar, Deverick J. Anderson, Barbara I. Braun, Philip Carling, Stuart Cohen, Curtis Donskey, Marci Drees, Anthony Harris, David K. Henderson, Susan S. Huang, Manisha Juthani-Mehta, Ebbing Lautenbach, Darren R. Linkin, Jennifer Meddings, Loren G. Miller, Aaron Milstone, Daniel Morgan, Sharmila Sengupta, Meera Varman, Deborah Yokoe, Danielle M. Zerr, on behalf of the Research Committee of the Society for Healthcare Epidemiology of America
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 35 / Issue 5 / May 2014
- Published online by Cambridge University Press:
- 10 May 2016, pp. 480-493
- Print publication:
- May 2014
-
- Article
- Export citation
-
This white paper identifies knowledge gaps and new challenges in healthcare epidemiology research, assesses the progress made toward addressing research priorities, provides the Society for Healthcare Epidemiology of America (SHEA) Research Committee's recommendations for high-priority research topics, and proposes a road map for making progress toward these goals. It updates the 2010 SHEA Research Committee document, “Charting the Course for the Future of Science in Healthcare Epidemiology: Results of a Survey of the Membership of SHEA,” which called for a national approach to healthcare-associated infections (HAIs) and a prioritized research agenda. This paper highlights recent studies that have advanced our understanding of HAIs, the establishment of the SHEA Research Network as a collaborative infrastructure to address research questions, prevention initiatives at state and national levels, changes in reporting and payment requirements, and new patterns in antimicrobial resistance.
Contributors
-
- By James Ahn, Eric L. Anderson, Annette L. Beautrais, Dennis Beedle, Jon S. Berlin, Benjamin L. Bregman, Peter Brown, Suzie Bruch, Jonathan Busko, Stuart Buttlaire, Laurie Byrne, Gerald Carroll, Valerie A. Carroll, Margaret Cashman, Joseph R. Check, Lara G. Chepenik, Robert N. Cuyler, Preeti Dalawari, Suzanne Dooley-Hash, William R. Dubin, Mila L. Felder, Avrim B. Fishkind, Reginald I. Gaylord, Rachel Lipson Glick, Travis Grace, Clare Gray, Anita Hart, Ross A. Heller, Amanda E. Horn, David S. Howes, David C. Hsu, Andy Jagoda, Margaret Judd, John Kahler, Daryl Knox, Gregory Luke Larkin, Patricia Lee, Jerrold B. Leikin, Eddie Markul, Marc L. Martel, J. D. McCourt, MaryLynn McGuire Clarke, Mark Newman, Anthony T. Ng, Barbara Nightengale, Kimberly Nordstrom, Jagoda Pasic, Jennifer Peltzer-Jones, Marcia A. Perry, Larry Phillips, Paul Porter, Seth Powsner, Michael S. Pulia, Erin Rapp, Divy Ravindranath, Janet S. Richmond, Silvana Riggio, Harvey L. Ruben, Derek J. Robinson, Douglas A. Rund, Omeed Saghafi, Alicia N. Sanders, Jeffrey Sankoff, Lorin M. Scher, Louis Scrattish, Richard D. Shih, Maureen Slade, Susan Stefan, Victor G. Stiebel, Deborah Taber, Vaishal Tolia, Gary M. Vilke, Alvin Wang, Michael A. Ward, Joseph Weber, Michael P. Wilson, James L. Young, Scott L. Zeller
- Edited by Leslie S. Zun
- Edited in association with Lara G. Chepenik, Mary Nan S. Mallory
-
- Book:
- Behavioral Emergencies for the Emergency Physician
- Published online:
- 05 April 2013
- Print publication:
- 21 March 2013, pp viii-xii
-
- Chapter
- Export citation
Contributors
-
- By C. Alan Anderson, Celso Arango, David B. Arciniegas, Igor Bombin, Robert W. Buchanan, C. Robert Cloninger, Joshua Cosman, C. Munro Cullum, Felipe DeBrigard, Steven L. Dubovsky, Robert Feinstein, Lynne Fenton, Christopher M. Filley, Laura A. Flashman, Morris Freedman, Oliver Freudenreich, Kimberly L. Frey, Lauren C. Frey, Kelly S. Giovanello, Deborah A. Hall, John Hart, Kenneth M. Heilman, Katherine L. Howard, Robin A. Hurley, Daniel I. Kaufer, Sita Kedia, James P. Kelly, B. K. Kleinschmidt-DeMasters, Benzi M. Kluger, David G. Lichter, Deborah M. Little, Deborah M. Lucas, Thomas W. McAllister, Mario F. Mendez, Doron Merims, Steven G. Ojemann, Fred Ovsiew, Brian D. Power, Bruce H. Price, Gila Z. Reckess, Martin L. Reite, Matthew Rizzo, Donald C. Rojas, Michael Henry Rosenbloom, Elliott D. Ross, Jeremy D. Schmahmann, Stuart A. Schneck, Jonathan M. Silver, Mark C. Spitz, Sergio E. Starkstein, Katherine H. Taber, Robert L. Trestman, Hal S. Wortzel
- Edited by David B. Arciniegas, C. Alan Anderson, Christopher M. Filley
-
- Book:
- Behavioral Neurology & Neuropsychiatry
- Published online:
- 05 February 2013
- Print publication:
- 24 January 2013, pp vii-x
-
- Chapter
- Export citation
Health in the Marketplace: Professionalism, Therapeutic Desires, and Medical Commodification in Late-Victorian London. ByTakahiro Ueyama. Palo Alto, Calif.: Society for the Promotion of Science and Scholarship, 2010. 320 pp. Cloth, $55.00. ISBN: 978-0-930664-29-9.
- Stuart Anderson
-
- Journal:
- Business History Review / Volume 86 / Issue 3 / Autumn 2012
- Published online by Cambridge University Press:
- 30 November 2012, pp. 607-610
- Print publication:
- Autumn 2012
-
- Article
- Export citation
Contributors
-
- By Waiel Almoustadi, Brian J. Anderson, David B. Auyong, Michael Avidan, Michael J. Avram, Roland J. Bainton, Jeffrey R. Balser, Juliana Barr, W. Scott Beattie, Manfred Blobner, T. Andrew Bowdle, Walter A. Boyle, Eugene B. Campbell, Laura F. Cavallone, Mario Cibelli, C. Michael Crowder, Ola Dale, M. Frances Davies, Mark Dershwitz, George Despotis, Clifford S. Deutschman, Brian S. Donahue, Marcel E. Durieux, Thomas J. Ebert, Talmage D. Egan, Helge Eilers, E. Wesley Ely, Charles W. Emala, Alex S. Evers, Heidrun Fink, Pierre Foëx, Stuart A. Forman, Helen F. Galley, Josephine M. Garcia-Ferrer, Robert W. Gereau, Tony Gin, David Glick, B. Joseph Guglielmo, Dhanesh K. Gupta, Howard B. Gutstein, Robert G. Hahn, Greg B. Hammer, Brian P. Head, Helen Higham, Laureen Hill, Kirk Hogan, Charles W. Hogue, Christopher G. Hughes, Eric Jacobsohn, Roger A. Johns, Dean R. Jones, Max Kelz, Evan D. Kharasch, Ellen W. King, W. Andrew Kofke, Tom C. Krejcie, Richard M. Langford, H. T. Lee, Isobel Lever, Jerrold H. Levy, J. Lance Lichtor, Larry Lindenbaum, Hung Pin Liu, Geoff Lockwood, Alex Macario, Conan MacDougall, M. B. MacIver, Aman Mahajan, Nándor Marczin, J. A. Jeevendra Martyn, George A. Mashour, Mervyn Maze, Thomas McDowell, Stuart McGrane, Berend Mets, Patrick Meybohm, Charles F. Minto, Jonathan Moss, Mohamed Naguib, Istvan Nagy, Nick Oliver, Paul S. Pagel, Pratik P. Pandharipande, Piyush Patel, Andrew J. Patterson, Robert A. Pearce, Ronald G. Pearl, Misha Perouansky, Kristof Racz, Chinniampalayam Rajamohan, Nilesh Randive, Imre Redai, Stephen Robinson, Richard W. Rosenquist, Carl E. Rosow, Uwe Rudolph, Francis V. Salinas, Robert D. Sanders, Sunita Sastry, Michael Schäfer, Jens Scholz, Thomas W. Schnider, Mark A. Schumacher, John W. Sear, Frédérique S. Servin, Jeffrey H. Silverstein, Tom De Smet, Martin Smith, Joe Henry Steinbach, Markus Steinfath, David F. Stowe, Gary R. Strichartz, Michel M. R. F. Struys, Isao Tsuneyoshi, Robert A. Veselis, Arthur Wallace, Robert P. Walt, David C. Warltier, Nigel R. Webster, Jeanine Wiener-Kronish, Troy Wildes, Paul Wischmeyer, Ling-Gang Wu, Stephen Yang
- Edited by Alex S. Evers, Washington University School of Medicine, St Louis, Mervyn Maze, University of California, San Francisco, Evan D. Kharasch, Washington University School of Medicine, St Louis
-
- Book:
- Anesthetic Pharmacology
- Published online:
- 11 April 2011
- Print publication:
- 10 March 2011, pp viii-xiv
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Contributors
-
- By Ashok Agarwal, Joseph P Alukal, Deborah J Anderson, Linda D Applegarth, Saleh Binsaleh, Elizabeth M Bloom, Karen E Boyle, Nancy L Brackett, Robert E Brannigan, James V Bruckner, Victor M Brugh, Ettore Caroppo, Grace M Centola, Aleksander Chudnovsky, Susan L Crockin, Fnu Deepinder, David M. Fenig, Aaron B Grotas, Matthew P. Hardy, Wayne J. G. Hellstrom, Stanton C Honig, Stuart S Howards, Keith Jarvi, Rajasingam S Jeyendran, William E Kaplan, Edward Karpman, Sanjay S Kasturi, Mohit Khera, Nancy A Klein, Dolores J Lamb, Jane M Lewis, Larry I Lipshultz, Kirk C Lo, Charles M Lynne, R. Dale McClure, Antoine A Makhlouf, Myles Margolis, Clara I. Marín-Briggiler, Randall B Meacham, Jesse N Mills, John P Mulhall, Alexander Müller, Christine Mullin, Harris M Nagler, Craig S Niederberger, Robert D Oates, Dana A Ohl, E. Charles Osterberg, Rodrigo L Pagani, Vassilios Papadopoulos, Joseph A Politch, Gail S Prins, Angela A Reese, Susan A Rothmann, Edmund S Sabanegh, Denny Sakkas, Jay I Sandlow, Richard A Schoor, Paulo C Serafini, Mark Sigman, Suresh C Sikka, Rebecca Z Sokol, Jens Sønksen, Miguel Srougi, James Stelling, Justin Tannir, Anthony J Thomas, Paul J Turek, Terry T Turner, Mónica H. Vazquez-Levin, Moshe Wald, Thomas J Walsh, Thomas M Wheeler, Daniel H Williams, Armand Zini, Barry R Zirkin
- Edited by Larry I. Lipshultz, Stuart S. Howards, University of Virginia, Craig S. Niederberger, University of Illinois, Chicago
-
- Book:
- Infertility in the Male
- Published online:
- 19 May 2010
- Print publication:
- 24 September 2009, pp vii-x
-
- Chapter
- Export citation
Pulsar Applications of the Caltech Parkes Swinburne Baseband Processing System
- Willem van Straten, Matthew Britton, Matthew Bailes, Stuart Anderson, Shri Kulkarni
-
- Journal:
- International Astronomical Union Colloquium / Volume 177 / 2000
- Published online by Cambridge University Press:
- 12 April 2016, pp. 283-284
- Print publication:
- 2000
-
- Article
-
- You have access Access
- Export citation
-
The Caltech-Parkes-Swinburne Recorder (CPSR) was installed at the Parkes Radio-telescope in August of 1998. It is capable of continuously two-bit quadrature-sampling a 20 MHz bandpass in two polarizations, though other configurations are possible. Since its successful installation, over 17 Terabytes of observational data have been recorded. These data were processed using the Swinburne Baseband Processing System (SBPS), a suite of data management and reduction software executed using a Beowulf-style cluster of high-performance workstations. A description of CPSR and SBPS is presented herein, followed by a brief presentation of some results from the past year of observations, and an outline of possible future uses of the system.
A New Major Seti Project Based on Project Serendip Data and 100,000 Personal Computers
- Woodruff T. Sullivan III, Dan Werthimer, Stuart Bowyer, Jeff Cobb, David Gedye, David Anderson
-
- Journal:
- International Astronomical Union Colloquium/ Volume 161 /
- Published online by Cambridge University Press:
- 01 January 1997, pp. 729-734
-
- Article
- Export citation
-
We are now developing an innovative SETI project, tentatively named seti@home, involving massively parallel computation on desktop computers scattered around the world. The public will be uniquely involved in a real scientific project. Individuals will download a Screensaver program that will not only provide the usual attractive graphics when their computer is idle, but will also perform sophisticated analysis of SETI data using the host computer. The data are tapped off Project Serendip IV’s receiver and SETI survey operating on the 305-meter diameter Arecibo radio telescope. We make a continuous tape-recording of a 2 MHz bandwidth signal centered on the 21 cm H I line. The data on these tapes are then preliminarily screened and parceled out by a server that supplies small chunks of data (50 sec of 20 kHz bandwidth, a total of 0.25 MB) over the Internet to clients possessing the screen-saver software. After the client computer has automatically analyzed a complete chunk of data (in a much more detailed manner than Serendip normally does) a report on the best candidate signals is sent back to the server, whereupon a new chunk of data is sent out. If 50,000-100,000 customers can be achieved, the computing power will be equivalent to a substantial fraction of a typical supercomputer, and seti@home will cover a comparable volume of parameter space to that of Serendip IV.